Light as medicine: Flashing lights found to halt Alzheimer’s disease
12/16/2016 / By David Gutierrez

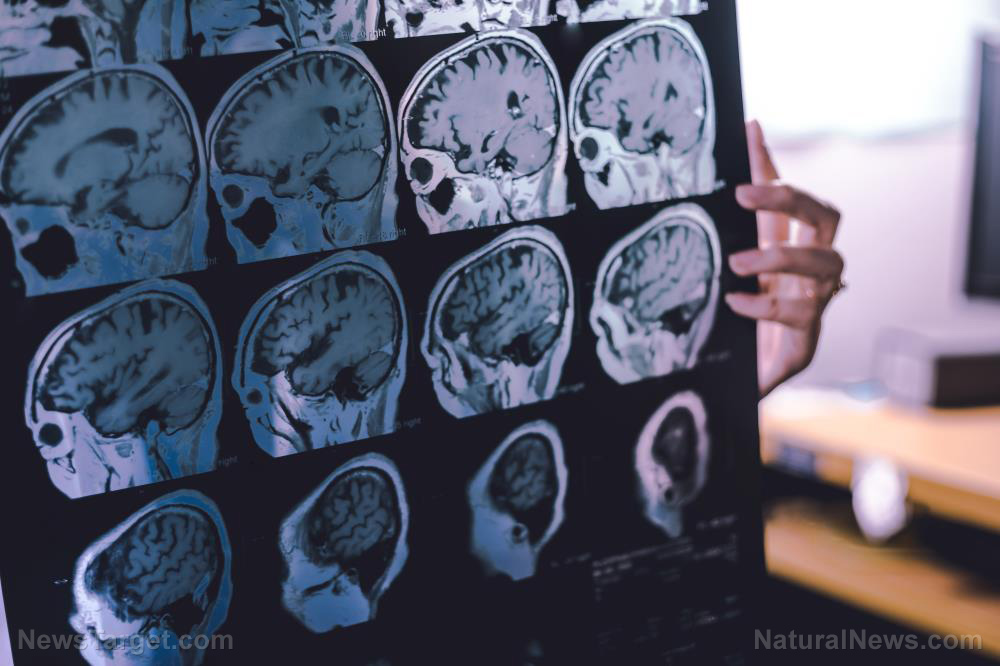
(NaturalNews) Lights flashing at a precise frequency might hold promise as a treatment for Alzheimer’s disease, according to a study conducted by researchers from the Massachusetts Institute of Technology, and published in the journal Nature.
Significantly, the treatment worked by activating the brain’s own dedicated immune system, causing the brain to clear out the amyloid plaques that are the physiological signature of the disease.
Alzheimer’s is the most common form of dementia, which is characterized by progressive decline in memory and cognitive function. No form of dementia has any known cure or effective treatment.
Dementia is now the top killer in the United Kingdom. In the United States, it ranks third behind heart disease and cancer. Worldwide, rates of dementia continue to rise.
Striking, but short-lived
Mice with amyloid plaques in their brains were exposed to LEDs flickering at a frequency of 40 Hz, the same frequency as the brain waves known as gamma oscillations. They found that in the visual cortex – one of the first areas to develop amyloid plaques in mice – levels of gamma oscillations immediately increased, accompanied by a dramatic increase in the activity of immune cells known as microglia, which play a key role in clearing debris from the brain.
The flicker is soft enough that it can barely be noticed by the human eye.
Within an hour, there were noticeable decreases in the amyloid concentrations in the treated mice’s visual cortexes. Overall, the concentration of amyloids decreased about 50 percent following treatment.
Within about a day, however, amyloid plaques had returned to their prior levels. So the researchers gave mice daily treatments with the LED box for a week. At the end of the week, they found that treated mice had amyloid levels 67 percent lower than untreated mice, and that their plaques were an average of 64 percent smaller.
Previously, the researchers had conducted a study that consisted of implanting LEDs into the brains of animals to see if an oscillating light could induce gamma oscillations. They focused on these oscillations because they are a type of brain wave that is significantly reduced in areas of the brain affected by Alzheimer’s. That study found that not only did the lights induce gamma oscillations, but they led to an increase in microglia activity.
The treatment was considered too invasive for human patients, however, so the researchers followed up with the new study.
Major hurdles remain
The major problem with the recent research is that the benefits of the light do not appear to have extended much beyond the visual cortex of the mice. But the human visual cortex does not tend to accumulate amyloid plaques; instead, these plaques concentrate in regions such as the hippocampus, which are believed to regulate cognition and memory.
Nevertheless, the researchers have formed a company, Cognito Therapeutics, that has already petitioned the FDA to begin trials in human Alzheimer’s patients.
“So many things have been shown to work in mice, only to fail in humans,” lead researcher Dr. Li Huei Tsai said. “But if humans behave similarly to mice in response to this treatment, I would say the potential is just enormous.”
If effective, the treatment may also have potential for other neuropsychiatric conditions characterized by reduced gamma oscillations, including autism, Parkinson’s disease and schizophrenia.
To date, no drugs targeting amyloid plaques have shown effectiveness in treating Alzheimer’s disease. But the researchers say that those interventions had either not acted early enough, or had not found an ideal method of affecting the plaque buildup.
“I think we have something very fundamentally different,” Tsai said.
Tsai noted that if it can be developed into a treatment, light therapy has the advantage of not needing to bypass the blood-brain barrier, as drugs do. As a non-pharmaceutical treatment, it is likely to have significantly fewer side effects.
Most significantly, Tsai emphasized that the treatment relies on the body’s own immune system, rather than an external agent.
“We just directly recruit other neurons and other cell types in the brain to sort of enable the brain’s inner ability to repair itself,” Tsai said.
Sources for this article include:
Tagged Under: Alzheimer's disease, dementia, immune system, microglia
RECENT NEWS & ARTICLES
COPYRIGHT © 2017 ALZHEIMERS NEWS